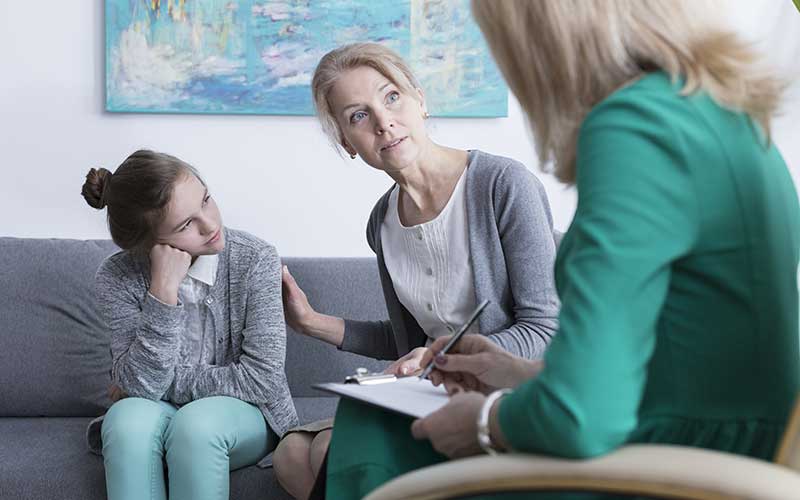by Michelle Yep-Martin, PsyD | Apr 7, 2021 | Behavioral Health Topics
I have always thought of myself as the kind of psychologist who offers a safe space for a patient to walk in, unload all that is bothering them out onto my carpet, and leave without a thought for me to clean up. Sometimes they continue to carry pieces with them, but with each additional session, we are able to get to the core of the issue together.
I am sure all of us would love to have a caseload of clients who come in on time, ready to work on their issues, make progress at a steady pace, and pay on time (preferably in cash!). Unfortunately, this is, for most of us, not a fact of life.
Continue Reading

by Clinton Nowicke, PsyD | Jan 21, 2021 | Behavioral Health Topics, Lifehacks, Tips & Advice
Typically, when therapists are asked to define “cultural competence” their response is usually race-based or location-based. Occasionally some include gender and sexual minorities, age, and ability. It’s rare that clinicians and therapists with little experience in deafness consider “Deaf” as a culture.
The topic of deafness and Deaf culture is vast, with many aspects to consider. It would be impossible to cover everything in only a few blog posts. This article is the first of a series about working with Deaf and Hard-of-Hearing (DHH) clients is intended as a starting point for clinicians to begin their own research into deafness and Deaf culture.
Continue Reading

by Katie Pesch, PhD | Nov 4, 2020 | Behavioral Health Topics
Almost all developing therapists move through a phase of resisting ambiguity. The uncertain, variable nature of psychotherapy can be intimidating and leave you feeling like a novice with every new challenging case. I often wish for a map that would help me guide my clients on their paths from suffering to contentment.
But there’s a reason ambiguity is inherent in this work: Psychotherapy is relational in nature. It is part theory, education, and research, and part human connection. The latter is the source of ambiguity that can be difficult to move into as a beginning therapist, but it’s also central to effective therapy.
Common factors research highlights the importance of the therapeutic relationship above and beyond specific theoretical orientations [1]. It provides empirical evidence that the therapist’s authentic human presence within the therapeutic relationship is a key factor of change.
Continue Reading

by Macy Wilson, PsyD | Oct 2, 2020 | Behavioral Health Topics
It seems that workplaces, schools, companies, and organizations are increasingly paying more attention to diversity and culture lately.
While this growing interest is encouraging, there are times when there is a significant lack of follow-through regarding the attention these issues receive. This is a disservice to everyone involved, but it comes at a special price in the realm of therapy.
I know of several graduate programs that pride themselves on their emphasis on diversity, yet have only a few course offerings specifically related to the topic and do not consistently revisit cultural issues throughout other courses.
With regard to psychology and therapy, the lack of consistent attention to cultural issues has the potential to create and maintain impasses that can affect the client’s progress.
As aspiring mental health professionals, we have the best of intentions in our work with clients. It is very important, however, to assess for cultural importance and issues of diversity in our first meetings with clients and then to be mindful of the ways we communicate with those clients moving forward.
Continue Reading

by Cameron Mosley, MS | May 22, 2019 | Behavioral Health Topics
You’ve heard about exposure therapy. Maybe you’ve been interested in trying it out with patients, but you don’t know enough about the procedure, or you’re worried it could do more harm than good. This guide will give you an overview of why exposure therapy can be beneficial to your patients, how to get started, and where to learn more.
Continue Reading

by Keeanna Powell, MS, LAPC | Sep 5, 2018 | Behavioral Health Topics, Lifehacks, Tips & Advice
So, tomorrow is your first session with a new client. First, congratulations! Every new client is a new opportunity to assist and provide support to someone along his or her journey. Whether this is your first session with a new client or the very first session of your career, it is completely understandable to feel nervous or experience jitters.
Fear of the unknown regarding new clients can be intense. You may be asking yourself questions similar to these as you prepare to meet your new client: Will I be able to help her? Will he like my therapeutic approach? What if he asks a question I can’t answer? Will she even show up? The following are some tips to help you prepare for your first session.
Continue Reading

by Dr. Nina Silander | Jun 26, 2018 | Behavioral Health Topics, Professional Resources
We are not always so good at saying goodbyes. There’s just something a bit uncomfortable about it. While we, as mental health professionals, obtain instruction and training in the nuances of communication and relationship, carrying out a solid, healthy therapeutic adieu with our clients requires some forethought, preparation, and skill. The following is a review of considerations and tips for terminating psychotherapy with success.
Continue Reading

by Dr. Nazo Shamal | Jun 19, 2018 | Behavioral Health Topics, Professional Resources
Treatment tracking is important because it gives you a baseline, and therapists can use repeated assessment to track progress and re-plot the course when things get off track.
Imagine walking into a therapist’s office seeking services to deal with a so-called problem or issue you have. You walk in with immense nervousness and torpidity, you feel you want it to be over before it even begins. You find yourself sitting on a sofa across from a stranger and all you’re thinking about is what you’re supposed to say or do.
But then, the stranger across from you starts to speak and describes an entire process of how therapy generally unveils. You hear about confidentiality, possible therapeutic styles and interventions, and length of treatment. You begin to feel a bit comfortable and start to relax. This information starts to ease your discomfort and the picture begins to appear clearer about what you’ve gotten yourself into.
Continue Reading

by Katie Arfa, PsyD, NSCA-CPT | May 24, 2018 | Behavioral Health Topics
Butterflies in your stomach. A gut-wrenching feeling. Your stomach suddenly drops… You’d better go with your gut.
I don’t know about you, but all of these phrases packed together gives me a general sense of unease, and for good reason. For most people, these sayings have become synonymous with the kind of scary, traumatic, or anxiety-provoking situations that simply make your stomach churn (pun intended).
On the other hand, for the positive psychology folks, we could also be talking about a remarkably exhilarating experience — falling in love, skydiving, riding a rollercoaster. There are endless scenarios that have elicited this reaction in our lives. But what do they all have in common?
Continue Reading
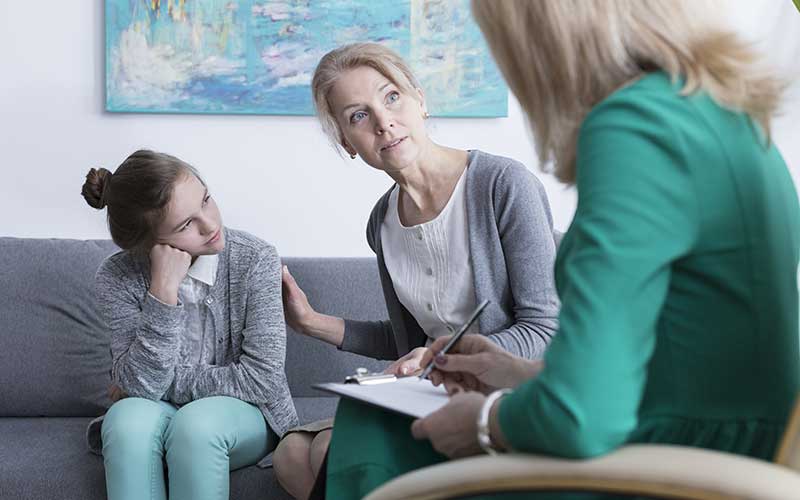
by Aaron R. Montgomery, PsyD | Feb 5, 2018 | Behavioral Health Topics, Professional Resources
One of the challenges I faced during my training as a psychologist was determining how to improve client behavior between sessions in order to optimize treatment outcomes.
Clients often presented with stressful family relationships, relationships that seemed to limit therapeutic progress. I wanted to help my clients as individuals, but I also understood that they did not exist within vacuums. In family therapy, I was able to help clients appreciate how family dynamics and communication styles are important factors in achieving their individual behavioral health goals.
Family therapy also extended my therapeutic reach beyond the individual and beyond the one hour that we had together each week.
Continue Reading