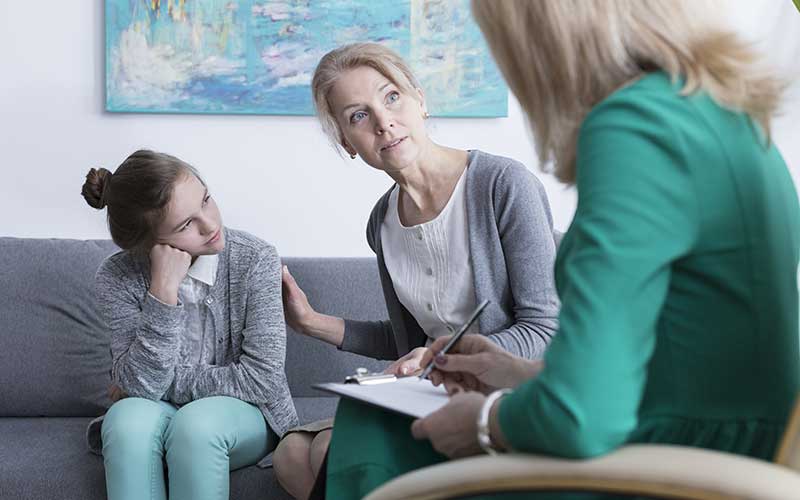by Todd Griffin | Mar 6, 2018 | Professional Resources, Self-Care
Therapists are the heroes of mental health — after all, they help people cope with their problems and be healthier mentally and psychologically. Without therapists, many people would have no idea how to deal with their respective issues. However, if you’re a therapist and you’re experiencing issues of your own, there is no shame in seeking the help of another therapist.
If you’re unsure whether you need another therapist’s help, or if you’re also a client who thinks your therapist may benefit from therapy, there are signs to look out for.
Continue Reading
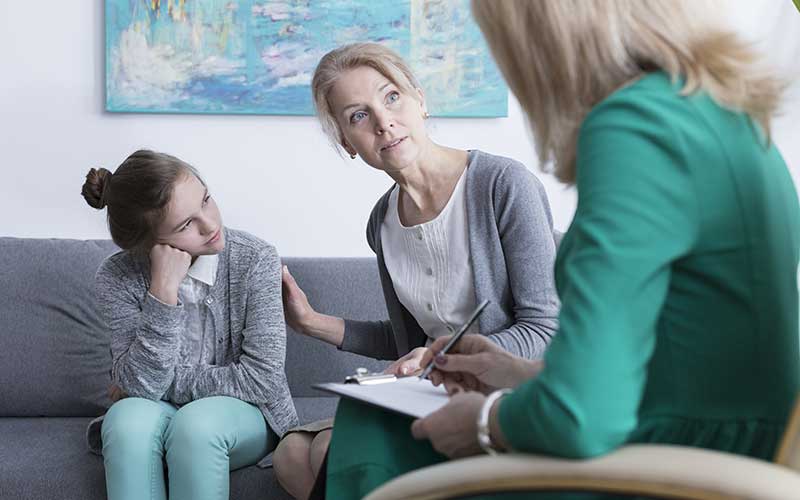
by Aaron R. Montgomery, PsyD | Feb 5, 2018 | Behavioral Health Topics, Professional Resources
One of the challenges I faced during my training as a psychologist was determining how to improve client behavior between sessions in order to optimize treatment outcomes.
Clients often presented with stressful family relationships, relationships that seemed to limit therapeutic progress. I wanted to help my clients as individuals, but I also understood that they did not exist within vacuums. In family therapy, I was able to help clients appreciate how family dynamics and communication styles are important factors in achieving their individual behavioral health goals.
Family therapy also extended my therapeutic reach beyond the individual and beyond the one hour that we had together each week.
Continue Reading

by Reina Remigio, PhD | Jan 29, 2018 | Professional Resources, Student & Intern Resources
The core purposes of clinical supervision are to protect the welfare of clients by ensuring they are receiving ethical, quality care and to promote the growth of pre-licensed clinicians [1].
A couple of main areas that distinguish pre-licensure clinical supervision from consultation, mentoring, or another form of guidance are the evaluative and non-voluntary components of the supervisory relationship [1].
This tends to amplify a supervisee’s existing anxiety related to questions of competency, training demands, and balancing academic, occupational, and personal obligations [2]. Too often, the level of anxiety is suboptimal, negatively impacting learning, growth, and clinical work.
Continue Reading

by Audrey Davidheiser, PhD | Jan 8, 2018 | Professional Resources, Student & Intern Resources
The #MeToo movement has exposed powerful men who leverage their positions to abuse and manipulate. The courage these women and men exhibit as they step forward to confront this behavior is inspiring.
May it continue to motivate other survivors to come forward, because as statistics show, roughly 2 out of 3 sexual assaults go unreported [1]. What a jarring reality, especially since nearly 1 in 5 women and 1 in 71 men reported experiencing rape at some time in their lives [2].
Survivors may have many reasons not to publicize their story. But if and when they do, are we as mental health providers prepared to help? A thorough manual on how therapists can propel them toward recovery is beyond the scope of this article [3], so what follows are 5 concepts to remember when working with survivors of sexual abuse.
Continue Reading

by Jon Weingarden, PsyD | Dec 22, 2017 | Behavioral Health Topics, Professional Resources
And there’s nothing you can do about it! You have to fail. You must fail… If you want to succeed.
To foster a patient who loves himself, warts and all, therapists must accept and own their foibles and follies. To the best of my knowledge, there is no greater strength than the courage to look our demons straight in the eye. This is a question – “what are your strengths and weaknesses?” – you will face at comprehensive exams and internship interviews; my answer always begins, “they are one-and-the-same: my greatest strength is how I have grown from my weaknesses.”
Continue Reading

by Sofie Champassak, Ph.D. | Dec 18, 2017 | Personal & Professional Experiences, Professional Resources, Uncategorized
The Examination for Professional Practice in Psychology (EPPP) is something every psychology graduate student dreads. After spending years in school, hours reading, writing, applying for internship and fellowship, and collecting clinical hours, the day has finally come for that very last step.
Of course, it’s normal to feel anxious about the EPPP. Many have said, “You feel like you’re failing it the whole time you’re taking it, but it will be fine.” Or there’s an optimistic tone of, “You’re going to be fine, you’ll do great! You just need a score of 500 to pass.”
Then there are the aftermath celebrations and Facebook updates: “I passed the EPPP!” Or, “Another step closer to being licensed!”
I found it so rare and uncommon for my peers to speak about the other possibility: What happens if you don’t pass?
Continue Reading

by Traci W. Olivier, Psy.D. | Dec 4, 2017 | Lifehacks, Tips & Advice, Professional Resources, Student & Intern Resources
The concept of resilience has become quite a popular one lately. There are countless articles, workshops, lectures, and even centers that focus on resilience.
But what exactly is it? And from where does it come?
Is it an inherited personality trait predetermined by genetics? Or is it something that can be taught, fostered, and developed? Perhaps more importantly, why do some people seem so much better at it than others?
These are exactly the kinds of questions that have inspired my colleague, Dr. Darlyne Nemeth, and me to probe deeper into the concept of resilience. Our research and experiences eventually transpired into a book, which was recently published.
We described the hallmark of resilient people as being grounded in today, learning how to benefit from yesterday, and imagining themselves in tomorrow. Resilience is not just about surviving, but also about thriving in the midst of challenge.
Continue Reading

by David C. Talavera | Nov 13, 2017 | Professional Resources
Despite the growing need for Spanish-language mental health services, there is a shortage of bilingual clinicians, as well as inadequate training for them [1,2].
Does this mean you have to brush up on your Spanish to provide Spanish-language services? Not necessarily.
Here are some helpful tips for working with Spanish-speaking patients if you don’t know Spanish. And if you do know Spanish but are hesitant to use it for clinical work, keep reading for tips to help make that transition as smooth as possible.
Continue Reading

by Eric Zhou, PhD | Oct 20, 2017 | Professional Resources
The EPPP: 4 letters that will strike fear in the hearts of clinical psychology graduates everywhere!
Developed and administered by the Association of State and Provincial Psychology Boards (ASPBB), the Examination for Professional Practice in Psychology is a 225-item test of endurance spanning 4.5 hours (including the 15-minute tutorial).
For many, the EPPP represents one of the last hurdles that must be tackled before they can hang up a shingle outside of their office doors and proudly proclaim themselves to be a licensed clinical psychologist.
Continue Reading

by Christina Wohleber, PsyD | Oct 16, 2017 | Professional Resources, Self-Care
Ever notice yourself getting a little more irritable than normal? Finding it difficult to interact with colleagues, clients, and even family or friends? Struggling to find empathy and patience for others? This could be the result of therapist burnout. Yes, even therapists get burned out and need to take a step back in order to take care of our own needs.
Therapist burnout happens when an individual’s psychological resources are overpowered by the demands placed on them. It is an extreme kind of exhaustion that can result from working with particularly challenging populations [1].
Not only does burnout cause us to simply feel terrible, but it also contributes to job dissatisfaction and poor job performance. Further, it can lead to frantic job searches, and, at the extreme end, it can result in ethical violations, which may have professional repercussions for the therapist – and may harm the client.
Continue Reading